




Pain is a universal human experience, yet its underlying science is often misunderstood. Whether fleeting or persistent, pain plays a critical role in alerting us to injury or disease. However, not all pain is the same, and understanding its complexities is vital for effective management. This article delves into the science of pain, with a special focus on neuropathic pain-a condition affecting millions worldwide. It aims to inform and empower by exploring its causes, symptoms and treatment options.
Pain begins as a signal in the nervous system, triggered when specialised nerve endings-called nociceptors-detect harmful stimuli. These signals travel along nerve fibres to the spinal cord and brain, where they are interpreted as pain. This process is known as nociception. Acute pain is typically short-lived and serves as a warning mechanism, prompting us to withdraw from danger. Chronic pain, on the other hand, persists for weeks, months, or even years, often outlasting its initial cause and becoming a health concern in itself.
The distinction between acute and chronic pain is crucial. Acute pain is usually linked to injury or surgery and resolves as healing occurs. Chronic pain can stem from ongoing conditions like arthritis or nerve damage and may not respond to conventional treatments. The brain’s interpretation of pain is influenced by emotional, psychological, and social factors, making pain a complex and multi-dimensional experience.
Neuropathic pain is a type of chronic pain that arises from damage or dysfunction in the nervous system, rather than from tissue injury alone. Unlike nociceptive pain, which results from physical harm, neuropathic pain is caused by abnormal signalling in nerves or the spinal cord. This pain can be severe, persistent, and difficult to treat, often described as burning, tingling, or shooting sensations. Neuropathic pain is estimated to affect between 7% and 10% of the population globally, making it a significant public health issue.
What sets neuropathic pain apart is its resistance to conventional painkillers and its tendency to persist even after the original injury has healed. It often leads to distress, sleep disturbances, and reduced quality of life, highlighting the importance of accurate diagnosis and targeted treatment.
There are many causes of neuropathic pain, ranging from common medical conditions to traumatic injuries. Diabetes is one of the leading causes, with high blood sugar levels damaging nerves over time-a condition known as diabetic neuropathy. Other causes include shingles (post-herpetic neuralgia), spinal cord injuries, multiple sclerosis, chemotherapy, and physical trauma to nerves.
The symptoms of neuropathic pain vary widely but often include burning or shooting pain, numbness, tingling, and heightened sensitivity to touch or temperature. Sometimes, even light pressure from clothing can trigger intense discomfort. Patients may also experience spontaneous pain without any obvious trigger, making daily activities challenging. Emotional distress, anxiety, and depression are common consequences, emphasising the need for holistic care.
Accurate diagnosis of neuropathic pain is essential for effective management. Clinicians begin with a thorough medical history and physical examination, focusing on nerve-related symptoms. They may use questionnaires, such as the DN4 or PainDETECT, to help distinguish neuropathic pain from other types.
Diagnostic tools include nerve conduction studies, electromyography (EMG), and imaging techniques like MRI or CT scans. These tests help identify nerve damage or underlying conditions. Blood tests may be used to rule out diabetes or vitamin deficiencies. Early diagnosis is crucial, as timely intervention can prevent worsening symptoms and improve outcomes.
The management of neuropathic pain often involves a combination of therapies. Medications are commonly prescribed, including anticonvulsants (such as gabapentin and pregabalin), antidepressants (like amitriptyline and duloxetine), and topical treatments (such as lidocaine patches). These drugs work by modulating nerve activity and reducing abnormal pain signals.
Physical therapy plays a vital role in promoting mobility and reducing pain. Techniques include stretching, strengthening exercises, and modalities such as heat or cold therapy. Psychological support, including cognitive behavioural therapy (CBT), helps patients cope with the emotional impact of chronic pain. Education and counselling empower patients to manage their symptoms and improve quality of life.
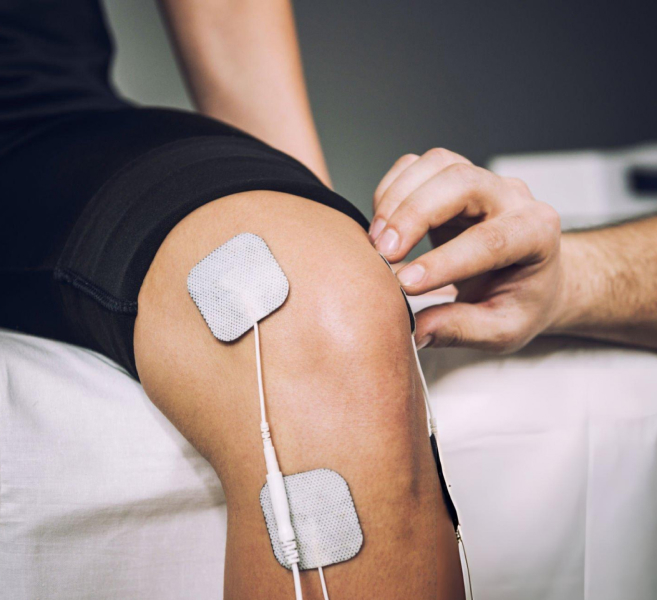
Advances in pain science have led to innovative therapies for neuropathic pain. Neuromodulation techniques, such as spinal cord stimulation and transcutaneous electrical nerve stimulation (TENS), use electrical impulses to alter pain signals. These methods are especially useful for patients who do not respond to medications.
Gene therapy is an exciting area of research, aiming to correct underlying genetic abnormalities or deliver pain-relieving molecules directly to nerve cells. Novel pharmaceuticals targeting specific pathways in the nervous system are in development, offering hope for more effective and personalised treatments.
Lifestyle interventions, including regular exercise, balanced nutrition, and stress management, are increasingly recognised for their role in pain control. Mind-body therapies, such as meditation and yoga, can reduce pain perception and improve overall well-being. Integrative approaches that combine traditional and emerging therapies may offer the best outcomes for patients.
Ongoing research is uncovering new insights into the mechanisms of neuropathic pain and potential treatment strategies. Scientists are exploring biomarkers for early diagnosis, advanced imaging techniques, and personalised medicine approaches. There is growing interest in developing drugs that target specific nerve receptors or inflammatory pathways.
Artificial intelligence and machine learning are being used to analyse patient data and predict treatment responses, paving the way for more tailored interventions. Collaboration between researchers, clinicians, and patients is vital to accelerate progress and bring new therapies to those in need. The future of pain management holds promise for improved quality of life and greater hope for those living with neuropathic pain.
Pain is a complex and multifaceted phenomenon, deeply rooted in the biology of the nervous system. Neuropathic pain, in particular, poses significant challenges due to its persistent nature and resistance to conventional treatments. Understanding the science behind pain and staying informed about emerging therapies is essential for patients and healthcare providers alike. With ongoing research and new treatment approaches, there is hope for better management and relief from neuropathic pain. By fostering awareness, education, and compassionate care, we can empower individuals to live fuller, healthier lives.
Spread the love, follow us on our social media channels