




Pain has a significant impact on our quality of life, movement, and overall well-being. Pain intervention therapies are our friends in such situations. It uses various techniques to manage our pain and help us go about our daily lives.
The good news is different methods of pain treatment not only help relieve discomfort but also target the root causes that cause the pain. Healthcare professionals can create personalised treatment plans by considering each patient’s specific needs and circumstances. This approach acknowledges that pain is influenced by various factors such as physical, emotional, social, and cognitive aspects.
Effective implementation of pain intervention therapies not only promotes enhanced patient outcomes but also contributes to reducing reliance on opioids or other less desirable solutions for managing pain.
Pain is a complex and subjective experience that can vary widely in its intensity, duration, and underlying causes. Understanding the different types of pain and their causes helps in developing effective pain intervention therapies. Pain can be broadly categorised into two main types:
Acute pain is usually short-lived and serves as a warning signal that something is wrong in the body. It often results from tissue damage, injury, or illness. Some common causes of acute pain include:
Chronic pain persists beyond the expected healing time and lasts for more than three to six months. It can be challenging to treat and may have a significant impact on a person’s quality of life. Some common causes of chronic pain include:
Pain intervention refers to a range of medical and therapeutic techniques utilised to manage and alleviate chronic or acute pain. These interventions do not seek to eliminate pain but rather provide individuals with the tools and strategies necessary to effectively cope with their pain.
Pain intervention can encompass various treatments such as medication management, physical therapy, acupuncture, nerve blocks, and psychological counselling. Each intervention is tailored to suit the specific needs of the individual and may be used in combination to achieve optimal results.
Furthermore, pain intervention can offer significant benefits beyond immediate relief by improving one’s overall quality of life and reducing the emotional distress that often accompanies chronic pain. By addressing both the physiological and psychological aspects of pain, it empowers individuals to regain control over their lives, fostering a sense of hope and empowerment that can greatly enhance well-being.
Non-invasive pain intervention therapies, such as acupuncture, massage, and chiropractic care, offer alternative or complementary approaches to pain management, eliminating the necessity for surgical procedures or medication. These therapies prioritise the enhancement of the body’s innate healing processes, while simultaneously improving circulation and alleviating tension.
Let us take a look at the most common non-invasive therapies:
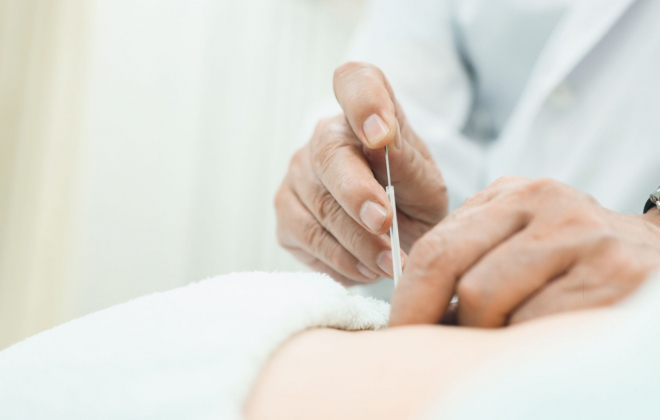
Acupuncture is a traditional Chinese medicine practice where thin needles are inserted into specific points of the body. These points are believed to be connected to energy pathways or meridians.
Acupuncture is thought to stimulate the body’s energy flow (qi) and promote balance. It has been traditionally used to treat various types of pain, including musculoskeletal, neuropathic, and chronic pain.
How It Works: Acupuncture is believed to stimulate the release of endorphins (natural pain-relieving chemicals) and affect the nervous system’s pain signalling. It may also influence inflammation and blood flow.
Effectiveness: Acupuncture has shown promising results in reducing pain, particularly for conditions like low back pain, osteoarthritis, migraines, and postoperative pain. However, its effectiveness can vary between individuals.
Risks and Side Effects:

Manipulating the muscles and soft tissues using various techniques, such as kneading, stroking, and applying pressure is known as massage. Apart from providing relaxation, massage can reduce muscle tension and improve circulation.
Massage therapy is commonly used to alleviate pain related to muscle tension, stress, and certain chronic conditions.
How It Works: Massage can increase blood flow to the treated area, release muscle knots, and trigger the body’s relaxation response. It may also have a positive impact on the release of endorphins.
Effectiveness: Massage therapy is effective for reducing pain associated with conditions like chronic lower back pain, fibromyalgia, and tension headaches. It can also improve overall well-being and quality of life.
Risks and Side Effects:
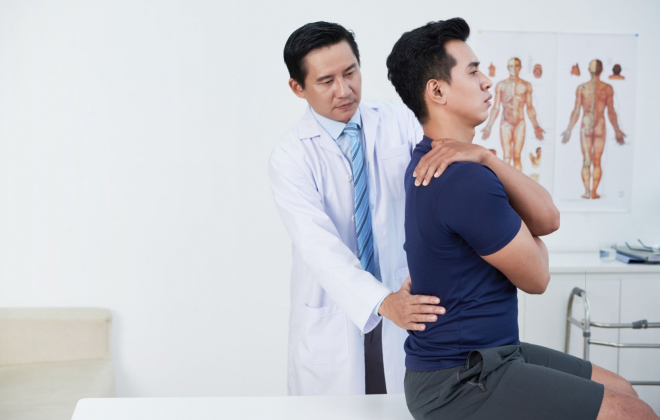
Chiropractic care involves manual manipulation of the spine and other joints to restore proper alignment and mobility. Chiropractors believe that misalignments (subluxations) in the spine can lead to pain and dysfunction.
Chiropractic adjustments aim to improve spinal alignment, alleviate nerve compression, and enhance overall body function.
How It Works: Chiropractic adjustments are thought to improve joint mobility, reduce inflammation, and promote the body’s natural healing mechanisms. They can also influence the nervous system’s pain signalling.
Effectiveness: Chiropractic care has shown promise in managing conditions like low back pain, neck pain, and headaches. However, the scientific evidence for its effectiveness is mixed, and it may not be suitable for all individuals.
Risks and Side Effects:
Invasive pain intervention therapies involve medical procedures that directly target the source of pain or disrupt pain signals. These interventions are typically considered when non-invasive treatments have not provided sufficient relief.
Let us take a look at three common invasive pain intervention therapies:
Nerve blocks involve the injection of a local anaesthetic, steroid, or other medications into or near a nerve or group of nerves to block pain signals. Nerve blocks can be used to diagnose the source of pain or provide temporary pain relief. There are different types of nerve blocks, including:
Nerve blocks interrupt the transmission of pain signals between the nerve and the brain, providing temporary relief. They can also have a diagnostic role in pinpointing the source of pain.
Epidural injections involve injecting a combination of anaesthetics and anti-inflammatory medications into the epidural space around the spinal cord. These injections can be used to manage pain in the back, neck, or legs and are commonly used for conditions like herniated discs, spinal stenosis, or radiculopathy.
Epidural injections reduce inflammation and pain around the spinal nerves. They can provide both diagnostic information and short- to medium-term pain relief.
Radiofrequency ablation is a minimally invasive procedure that uses radiofrequency energy to create heat and destroy a portion of a nerve responsible for transmitting pain signals. RFA is typically used for chronic pain conditions, such as arthritis-related pain or facet joint pain.
RFA heats the targeted nerve, disrupting its ability to transmit pain signals. The effects of RFA can last for several months, providing longer-term pain relief.
Invasive pain interventions are generally performed by trained medical professionals, such as pain management specialists, anaesthesiologists, or interventional radiologists. These procedures carry potential risks and benefits, and the decision to undergo such interventions should be made after a thorough discussion with a healthcare provider. It is essential to have a comprehensive evaluation and accurate diagnosis before considering any invasive pain intervention.
In medication-based pain intervention therapies, a group of medicines are prescribed to the patients, which work through different mechanisms to provide relief and improve the overall quality of life for individuals experiencing pain. The three most commonly used medication groups for this kind of therapy are:
Opioids are a class of medications that are derived from opium or synthetically produced to mimic opium’s effects. They are powerful pain relievers and are often used for severe or chronic pain. Opioids work by binding to opioid receptors in the brain and spinal cord, blocking pain signals and producing a sense of euphoria.
Types and Examples: Common opioids include morphine, oxycodone, hydrocodone, and fentanyl.
Considerations: Opioids can be effective for managing severe pain but also carry a risk of tolerance, dependence, and addiction. They are generally reserved for cases where other treatments have not provided adequate relief and are closely monitored by healthcare providers.
Risks and Side Effects:
NSAIDs are a group of medications that reduce pain, inflammation, and fever by inhibiting enzymes involved in the production of prostaglandins, which contribute to pain and inflammation. They are commonly used for various types of pain, including musculoskeletal and inflammatory conditions.
Types and Examples: Common NSAIDs include ibuprofen, naproxen, and aspirin.
Considerations: NSAIDs can be effective for short-term pain relief but may have potential side effects, including gastrointestinal irritation, ulcers, and increased risk of bleeding. Long-term use should be managed carefully, especially in individuals with pre-existing health conditions.
Risks and Side Effects:
Certain types of antidepressant medications are used to manage chronic pain, particularly neuropathic pain and certain types of musculoskeletal pain. These medications affect the levels of neurotransmitters in the brain, which can impact pain perception and mood.
Types and Examples: Tricyclic antidepressants (e.g., amitriptyline), selective serotonin and norepinephrine reuptake inhibitors (SNRIs, e.g., duloxetine), and certain atypical antidepressants (e.g., venlafaxine) are often used for pain management.
Considerations: Antidepressants can help manage chronic pain by affecting the nervous system’s pain signalling and enhancing the body’s natural pain-relieving mechanisms. They may take some time to show their full effects and can have side effects related to mood and cognition.
Risks and Side Effects:
Managing pain with medication requires the involvement of a qualified healthcare professional. The choice of medication depends on factors such as the type and severity of the pain, the person’s medical history, and any other medications they may be taking. Healthcare providers carefully assess the risks and benefits of different interventions to ensure effective pain management while minimising side effects or complications.
Pain intervention therapies allow you to get back on your feet. Effective pain management is crucial for improving quality of life, promoting well-being and maintaining daily activities. Pain, whether short-term or long-term, affects physical, emotional, and social aspects. Implementing proper approaches can bring relief and restore a sense of control over one’s health.
Open communication, collaboration, and a patient-centred approach are important aspects of successful pain management. By working together, patients and healthcare providers can develop personalised strategies that can enhance health and well-being.
Sources
Spread the love, follow us on our social media channels