



In a world where people are still learning about different health conditions, osteoarthritis remains one of the most common yet misunderstood conditions. Characterised by joint pain, stiffness, and reduced mobility, osteoarthritis affects millions worldwide.
However, with proper understanding and management, individuals can lead fulfilling lives despite their challenges. In this comprehensive guide, we explore various aspects of osteoarthritis, providing insights into its causes, symptoms, diagnosis, treatment options, and lifestyle modifications.
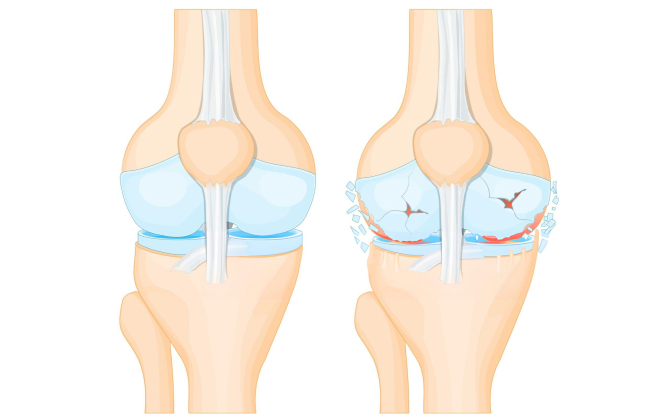
Osteoarthritis, often referred to as OA, is a degenerative joint disease that primarily affects the cartilage-the protective tissue covering the ends of bones within joints.
As the cartilage wears down over time, bones may begin to rub against each other, leading to pain, inflammation, and reduced flexibility.
While OA can affect any joint, it commonly occurs in the knees, hips, hands, and spine.
The exact cause of osteoarthritis remains elusive, but several factors contribute to its development. These include:
Symptoms of osteoarthritis typically develop gradually and worsen over time. Common signs include joint pain, stiffness, swelling, reduced range of motion, and tenderness in affected areas.
At first, you might notice some discomfort or mild pain when moving the affected joint, which can worsen over time. Stiffness typically occurs after periods of inactivity or rest and can make it challenging to move or use the joint properly. Swelling and tenderness may also be present due to inflammation in the joint.
As osteoarthritis progresses, you may experience a decreased range of motion in the affected joint as a result of cartilage damage.

In general, osteoarthritis is diagnosed through:
The healthcare provider will begin by gathering information about the patient’s medical history, including any symptoms they are experiencing, previous injuries or surgeries, family history of arthritis, and lifestyle factors that may contribute to joint issues.
A thorough physical examination is conducted to assess the affected joints. The healthcare provider will look for signs of swelling, tenderness, warmth, and joint deformities. They may also evaluate the range of motion and stability of the joints.
Imaging tests are commonly used to visualise the affected joints and assess the extent of damage. These may include:
In some cases, the healthcare provider may perform a procedure called arthrocentesis to aspirate fluid from the affected joint. The fluid can be analysed for signs of inflammation, infection, or other abnormalities.
While there are no specific blood tests to diagnose osteoarthritis, certain blood tests may be ordered to rule out other types of arthritis, such as rheumatoid arthritis or gout.
Osteoarthritis is typically diagnosed based on a combination of symptoms, physical examination findings, and imaging results. There are no specific laboratory tests that definitively diagnose osteoarthritis, so the diagnosis is primarily clinical.
While there is no cure for osteoarthritis, various treatment modalities aim to alleviate symptoms, improve joint function, and enhance overall quality of life. Treatment strategies may include:

In addition to medical interventions, adopting healthy lifestyle habits can significantly impact the management of osteoarthritis. These include:
Living with osteoarthritis presents challenges, but it does not define one’s life. With the right mindset, support system, and proactive approach to self-care, individuals can thrive despite the presence of this disease. Embracing adaptive strategies, seeking professional guidance, and prioritising overall well-being contribute to a fulfilling life journey.
Remember, while osteoarthritis may alter life’s course, it does not diminish one’s capacity for joy, purpose, and vitality.
Sources:
Spread the love, follow us on our social media channels