




Tuberculosis (TB) is a serious infectious disease that affects millions of people worldwide. Despite efforts to eradicate it, TB continues to be a major health concern.
In this article, we endeavour to understand TB in more detail. We will explore the causes, symptoms, diagnosis, and treatment of tuberculosis, as well as discuss the historical background and current challenges associated with this disease.

Tuberculosis has a long and storied history, often referred to as the “white plague” due to its terrible effects on populations throughout the centuries.
The roots of TB can be traced back to ancient Greece. About 25% of all deaths from the 1600s to 1800s were caused due to TB.
The disease has left an indelible mark on literature, art, and public health, with notable figures like Kafka and Chopin succumbing to its grasp.
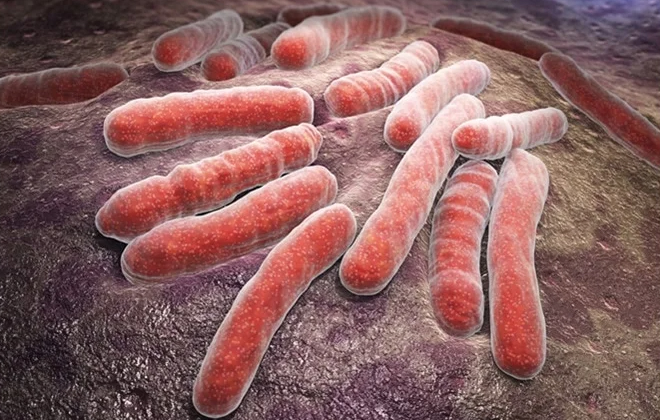
The causes of tuberculosis involve factors related to the transmission of the bacteria and conditions that increase the risk of infection. Tuberculosis is caused by a bacteria called Mycobacterium tuberculosis.
The result is a serious respiratory illness that can spread through the air when an infected person coughs or sneezes. The bacteria usually attack the lungs, but it can also affect other parts of the body such as the kidneys, spine, and brain.
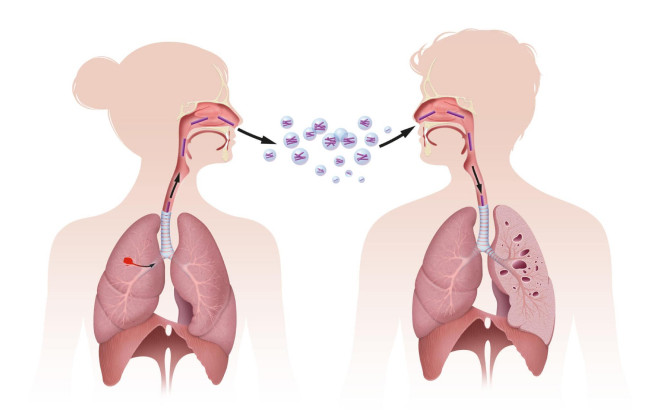
Tuberculosis can spread through one of these processes:
There are two forms of Tuberculosis – Latent TB and Active TB. Latent TB occurs when someone is infected with the TB bacteria but doesn’t show symptoms. The immune system keeps the bacteria in check, but there is a risk of it becoming active, especially if the immune system weakens.
Active TB, on the other hand, shows symptoms such as cough, chest pain, fatigue, weight loss, and fever. The immune system can’t control the bacteria, and the disease progresses. Active TB is contagious, while latent TB isn’t. It’s important to differentiate between the two for appropriate treatment.
Here are some of the common symptoms of the disease:

Tuberculosis is usually diagnosed through:
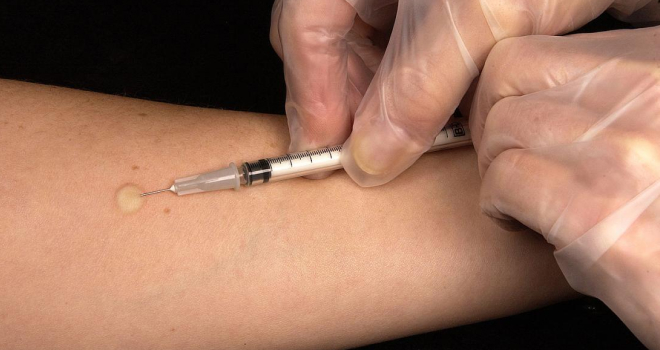
The Tuberculin Skin Test (TST) and Interferon-Gamma Release Assays (IGRAs) are used to detect latent tuberculosis infection. TST involves injecting a small amount of TB protein into the skin and checking for a reaction after 48-72 hours. IGRAs measure the release of a certain protein by T cells in response to TB antigens.
Compared to TST, IGRAs are more specific and not affected by prior vaccinations. Both tests help identify individuals with latent TB infection and guide decisions on preventive treatment. The choice between TST and IGRAs depends on factors like patient history and local epidemiology.
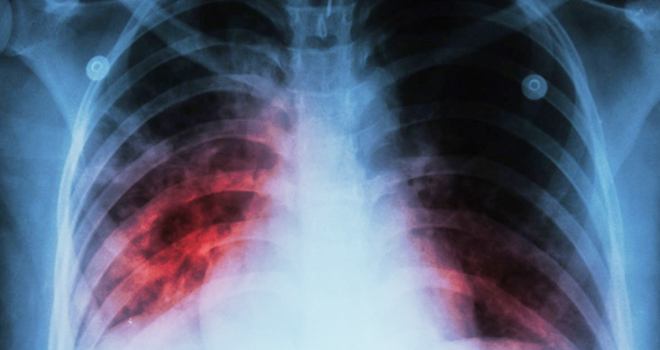
Chest X-rays and molecular diagnostics are essential in diagnosing tuberculosis. They show lung abnormalities and detect the genetic material of the bacteria.
Chest X-rays help identify the extent of infection and guide treatment decisions, while PCR provides a quick and accurate diagnosis.
The combination of these two techniques improves the efficiency of diagnosing tuberculosis, leading to better outcomes for patients.
In most cases, the treatment path includes:
First-line antitubercular drugs, including isoniazid, rifampin, ethambutol, and pyrazinamide, are essential in treating tuberculosis. These medications work together to disrupt bacterial cell wall synthesis, RNA synthesis, cell wall formation, and bacterial metabolism. This combination, known as DOTS, is crucial for successful treatment and prevention of drug-resistant strains. Administered over at least six months, these drugs play a key role in the global effort to control and eradicate TB.
Directly Observed Therapy (DOT) is a crucial tuberculosis (TB) treatment strategy where healthcare professionals or trained observers supervise patients as they take their medication daily to ensure adherence, prevent treatment failure, and decrease the development of drug-resistant TB strains. DOT is particularly beneficial for patients facing challenges in self-administration or adherence due to socioeconomic factors, ultimately leading to better treatment success and effectiveness in TB control programmes.
Drug-resistant tuberculosis (TB) is a major global health challenge caused by resistance to key antibiotics. Multidrug-resistant TB (MDR-TB) is resistant to at least two main drugs, while extensively drug-resistant TB (XDR-TB) is resistant to even more drugs. Factors like incomplete treatment and patient non-compliance contribute to the rise of drug-resistant strains. Treatment of drug-resistant TB requires specialised protocols with potentially toxic and less effective drugs. To combat this issue, improved diagnostics, treatment access, and public health interventions are necessary to prevent further spread of resistant strains.

Tuberculosis remains a formidable global health challenge that requires continued attention and concerted efforts. Understanding the causes, symptoms, diagnosis, and treatment options is vital for both healthcare professionals and the general public.
By fostering awareness, promoting early diagnosis, and advocating for increased resources, we can collectively work towards a future where tuberculosis is no longer a prevalent threat to public health.
Sources:
Spread the love, follow us on our social media channels